What is the purpose of this genetic research study?
The goal of this research study is to identify mutations in genes and regulatory elements on chromosomes that contribute to keloid scars. If we know what causes keloids in the first place we can study what makes cells in keloid scars malfunctioning. Better knowledge of how keloids form is necessary to develop better treatments.
About the Keloid Study
What are keloids?
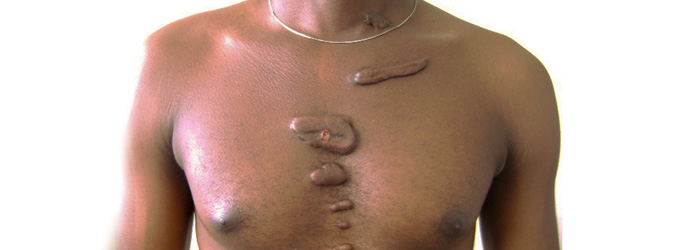
Keloids are scars that keep growing beyond the border of the original wound. They typically persist for several years, expand for an extensive period of time and are sometimes called benign tumors. Keloids often have a lumpy surface and are often tender, itchy or inflamed around the growing border.
Keloids can develop after surgery, injuries, ear piercing, vaccinations, acne or minor scratches. Keloids develop after injuries to the skin of most body parts but are rare on the palm of the hand or the sole of the foot. They do not occur in the mucosa of the mouth.
Some scars are bumpy and raised for several months but do not grow beyond the margin of the wound. Those are called hypertrophic scars and are not keloids. The distinction between small keloids and hypertrophic scars can sometimes be difficult.
Who can get keloids?
Keloids are most common in individuals of African ancestry but are also found in Asians and less frequently in Caucasians. Although there are no reliable numbers available, we estimate that approximately 1% of individuals of West African origin have keloids.
Young children and older adults rarely get keloids. It appears that most new keloids develop after puberty to the age of 30 or 40 years old.
Can keloids be inherited?
In most patients keloids do not run in the family. We believe that in the U.S. only about 1% of keloid cases are inherited. The way keloids are inherited is not yet clear (mode of inheritance). In the hereditary form of keloids it is possible that there is one major gene mutation that puts family members at risk for developing keloids. There may be other variations in the DNA (DNA makes up the chromosomes) that determine whether keloids become large and aggressive or stay small and without many symptoms. It is unknown whether the environment (food or the things one does) have an effect on keloids.
Those keloid patients who have no other keloid formers in their family are unlikely to pass the keloids on to their children. However, it cannot be excluded that their offspring have an increased risk to develop keloids. Most likely several minor mutations (variants) in the genome are necessary to cause those keloids.
Do we treat keloids?
No, we do not treat keloids. We perform basic research to understand the cause for keloids. Based on this knowledge we expect that better treatment can be developed in the future.
Why should I participate in such a genetic study?
While we have some knowledge on proteins that are produced at the wrong time or the wrong amount in keloid scars, we do not know what causes keloids in the first place. Some genes are suspected to be involved in keloid formation, but no mutation is known. We need the participation of a large number of keloid patients to solve this problem with the latest genetic methods that are available to us.
Your participation will help to reach our goal.
Will I directly benefit from this study?
You will not directly benefit from the results of this study. Our research contributes to the understanding of keloids, which you (or your child) or some of your (or your child’s) family members may have, as well as to the understanding of basic processes in wound healing.